Analysis of difficult-to-treat psychosis: Clinical pharmacology and functional pharmacogenetics |
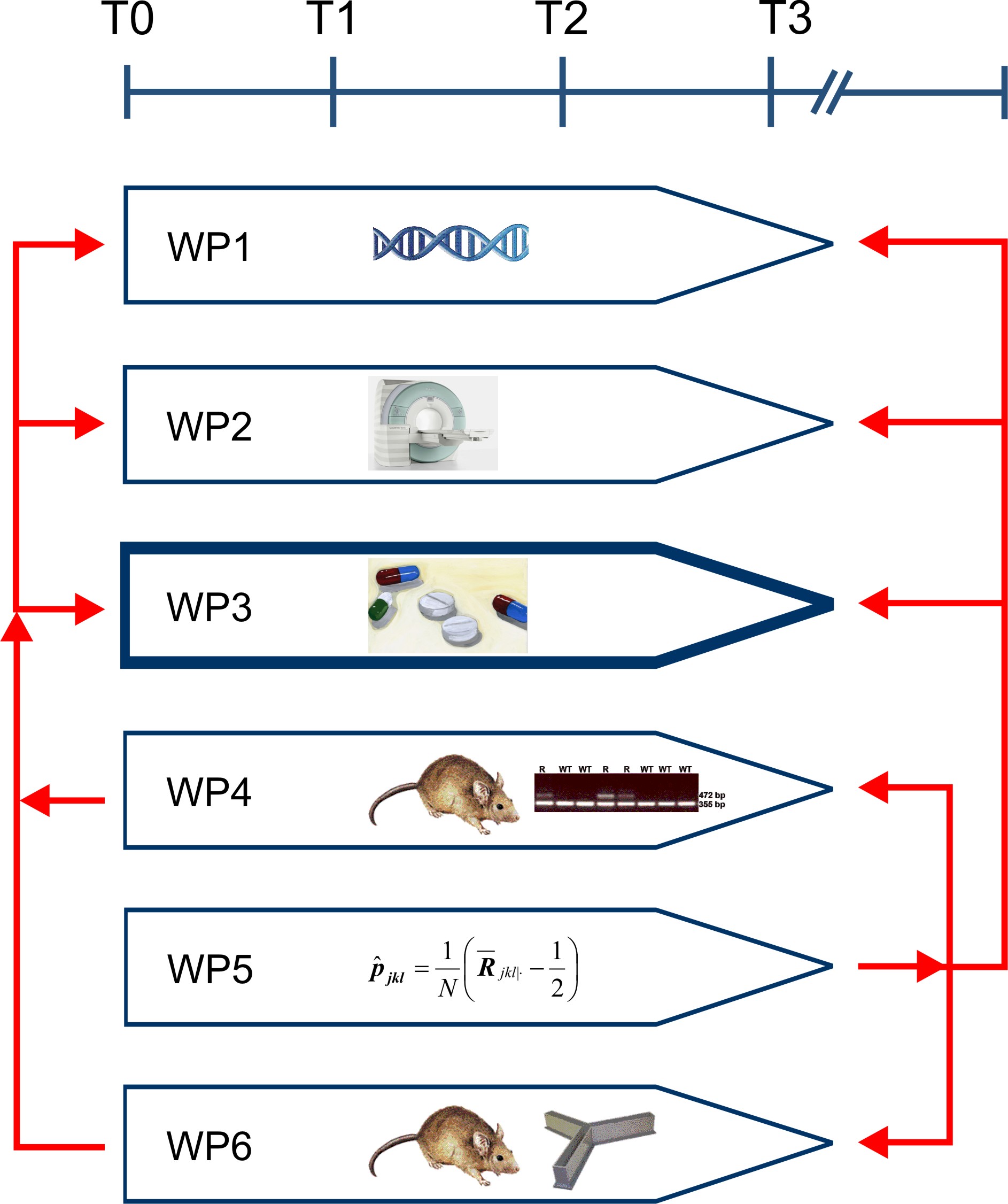
There is a significant fraction of difficult-to-treat patients with poor response to antipsychotics or mood stabilizers. We want to identify genetic determinants of these difficult-to-treat psychoses. Our project is divided into a clinical pharmacological and clinical pharmacogenetic approach on one side and an experimental functional pharmacogenetics approach on the other side.
The experimental approach concentrates on variation in genes responsible for membrane transport and biotransformation of antipsychotic drugs. Within the first 3 years, we study an anticipated number of 400 difficult-to-treat patients in comparison with a similar number of appropriate controls.
We similarily analayze the subgroup of patients poorly responding to therapy from WP1.
The functional pharmacogenetics approach focuses on membrane transport and metabolism of antipsychotic drugs and mood stabilizers in the gut, liver, and particularly at the blood brain barrier and in neuroglia cells. This serves to identify the influx and efflux transporters relevant for the antipsychotics and mood stabilizers. In the clinical samples, their naturally occurring variants are to be identified and functionally analyzed in model cell lines. We statistically analyze interactions between multiple proteins and their variants in the clinical samples and experimentally in multiple transfected cell lines.
Furthermore, at the moment we are establishing a clinicalpsychopharmacological/ pharmacogenetics expert unit serving both patient care and research.